A client emailed me last week complaining about her Medicare Advantage plan. She said her doctor gave her a prescription for Zolpidem, a sleeping pill, and her Medicare Advantage plan said they won’t pay for it.
Cora says the pharmacist at Walgreens can’t understand why Health Net refuses to cover Zolpidem. Cora’s doctor went the extra mile to put in a special request for this drug, but Health Net still refused to cover the drug. This is just a one-time prescription for Cora to take on a trip to Asia. Cora says she has trouble sleeping when crossing so many time zones, so she asked her doctor for a sleep aid.
Cora is mad at Health Net. I called the Health Net Pharmacy Department and asked why Cora is having a problem getting her Zolpidem. Here’s what I was told:
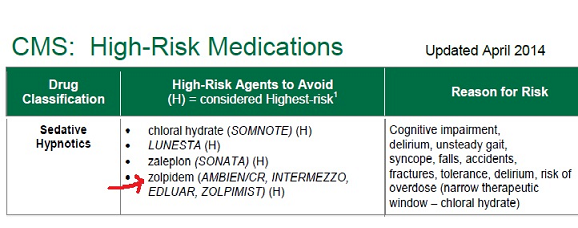
Zolpidem is on a CMS (Centers for Medicare and Medicaid Services) list of high risk drugs and they don’t think people over 65 should use it. Health Net says there are other, safer drugs Cora can use such as Temazepam, Trazodone, and Rozerem.
I did a Google search on Zolpidem and found a study that showed many people on this drug ended up falling and breaking hips. I also found the CMS list of high risk drugs people should not be taking.
So it turns out Health Net is not trying to give Cora and her doctor a hard time. They are following Medicare guidelines to protect Cora’s health.
But why doesn’t Walgreens pharmacist know about the CMS list of high risk drugs? And why doesn’t Cora’s doctor know about this? And why would Cora’s doctor prescribe a powerful drug when Cora could probably just buy a sleeping pill without a prescription?
The full list of high risk medications can be found here: http://www.priorityhealth.com/provider/clinical-resources/medication-resources/~/media/documents/pharmacy/cms-high-risk-medications.pdf